|
It’s been 28 days since I went under the knife, er, scalpel. Time has passed in a weird mixture of jumbled speed and staggering slowness, depending on which degree of pain you happen to be involved with at the time.
It started very suddenly, just a small pop at the same time as I coughed. This definitely wasn't a normal occurrence. I tried to forget about it, but there was a bit of discomfort after that and after a couple more weeks it seemed a good thing to pay a doctor visit. |
Doc Jargon: Repair & recovery
A young technician with a pleasant face but ruthless fingers seemed to find the spot in my abdomen that hurt. I asked her if she saw anything on the computer synced to the tool she was using, and she informed me she wasn't allowed to divulge information. Then, deadpan, she asked if I'd seen my doctor. “Yes,” I answered. “Did he mention ‘hernia,’ by any chance?” So then I knew.
Return visit to the doc. Now he told me it was an inguinal hernia. I’d never heard of such a thing. He explained I could choose to ignore it. It would never go away. There was a strong possibility it could strangulate, and that creates a life threatening situation. Or I could opt for surgery. The recovery period for the latter would be at least six weeks.
“Never go away, life-threatening, and recovery”, are powerful words when you’re making decisions about surgery. You tend to think mainly about the surgery itself, and you think, “well, if I go through that okay, the rest should be a snap.” So my decision was quick. Surgery took place just four months later.
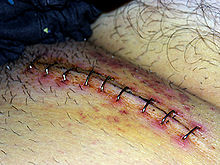 Source for text and pic: https://en.m.wikipedia.org/wiki/Inguinal_hernia
Source for text and pic: https://en.m.wikipedia.org/wiki/Inguinal_hernia
There are various surgical strategies which may be considered in the planning of inguinal hernia repair. These include the consideration of mesh use (e.g. synthetic or biologic), open repair, use of laparoscopy, type of anesthesia (general or local), appropriateness of bilateral repair, etc. Laparascopy is most commonly used for non-emergency cases, however, a minimally invasive open repair may have a lower incidence of post-operative nausea and mesh associated pain.
During surgery conducted under local anaesthesia, the patient will be asked to cough and strain during the procedure to help in demonstrating that the repair is without tension and sound.[16] Constipation after hernia repair results in strain to evacuate the bowel causing pain, and fear that the sutures may rupture. Opioid analgesia makes constipation worse. Promoting an easy bowel motion is important post-operatively.”
The in part
Surgical staff will confirm several times before your operation which side it’s on, and the surgeon himself confirms with you prior to him doing his work. He draws a pretty guide on you, then nurses cover your abdomen with a pink antiseptic fluid. The surgeon remarked I was pretty in pink. Remember the awful iodide stuff they used to use? Not any more. This stuff washes off the first time you have a shower.
The anaesthetist was wonderful, and we chatted for about an hour during the surgery. They gently put a sort of blue screen over my face, so I couldn't see what was happening, and I certainly couldn't feel it.
Afterwards I found myself in recovery room. I was in a sort of dazed state, but they kept me there, covered in warm blankets until I was with it enough to drink and even eat a cookie. I dressed, and was delivered to my dearly beloved. We walked all the way to the car. I felt wonderful. “Amazing!” I gloated.” I feel nothing! I'm just going to pick up where I left off!” The euphoria lasted until several hours later. Then, in spite of Tylenol 3’s, I found myself descending into a foggy sort of intense pain.
The out part--Ai! Yi! Yi!
Day 1: Surgery. felt fantastic, thought I'd be able to do anything. Went to bed
Day 2: Woke about 2 am. Huge pain whenever I moved. Couldn't get out of bed. Spent about 10 minutes struggling. Spent all day on the recliner chair except for bathroom breaks. Terrible pain, crying out when sitting or standing up with assistance.
Most useful thing...a recliner chair, pillow in the small of your back, another under your knees. Definitely someone to help you in your struggles to get up and down. When they do. be sure to focus on pushing a pillow hard into the wound area. It helps.
Day 3: Doubled up on the pain meds. Moaning instead of crying out with pain. Pain much better managed, but a bit dizzy from the meds. Still needed assistance, but tried slowly to wiggle myself forward, then push up to rise. Sitting still very painful.
Most helpful hint...don't wait until the pain grabs you. Take it as prescribed.
Day 4: Managing to sit and stand on my own. Huge feeling of freedom. Now practicing to rise and sit, many times. Squats using a chair back. Walking every time I get up, constipation becoming an uncomfortable problem, nothing happening.
Most helpful strategy. Before undergoing the surgery, take a stool softener a couple of days beforehand. Metamucil is also very helpful, even if yucky tasting. Eat some prunes and other dried fruit. Keep to this all through your recovery.
Day 5: Bowel problem solved! Huge relief. Standing and sitting much better. Lots of walking, but have to be careful, because I keep feeling a bit dizzy when up for very long.still not sleeping in bed.
Helpful hint...don't try to do too much.
Day 6: Noticed some bright red blood and pus on my dressing this morning. Feeling very weak and not enthused about doing anything. I'd decided yesterday I probably didn't need any more medications. Wrong!
Day 7, 8, 9, 10: I started to develop a routine, incorporating more and more household tasks, getting out into the garden, and, very blessedly, being helped by neighbors and dearly beloved along the way. On the eleventh day my GP checked the wound, and removed the 10 staples holding the outside skin.
Helpful hint...walking is great, and progressive gentle activity. Never strain, including when on the toilet. You don't want a repeat surgery experience, and there are lots of interior stitches that are still healing.
Day 28: One month later and recovery continues uneventfully. I do what I can, but don't force anything. I'm driving, sleeping in bed now, although still needing a pressure pillow against my side. A very active day will bring the need for pain medication in the evening, and I take it before the pain increases.
This morning I celebrated my first day able to pull some weeds from the raised beds and do a bit of planting winter veggies. WooHoo!
Final notes
It's worth doing your utmost to recover from inguinal surgery in a sensible way. A strangulated hernia of this type is life threatening.

 RSS Feed
RSS Feed


